The Arteries
of Innovation 2025 Annual Report
Message from the Co-Directors
“ The quality of our thinking cannot be higher than the quality of the information on which it is based.”

Justin
Ezekowitz,
MBBCh, MSc

Shaun
Goodman,
MD, MSc

Padma
Kaul,
PhD
In writing Thinking, Fast and Slow, Daniel Kahneman contemplated how we use information and the importance of the quality of data; low quality data will be unreliable from which to draw conclusions. The corollary of ‘garbage in, garbage out’ is that truth does not come from misinformation. Likewise, no matter how well a scientific story is “told”, testing the quality of the information in further studies remains paramount.
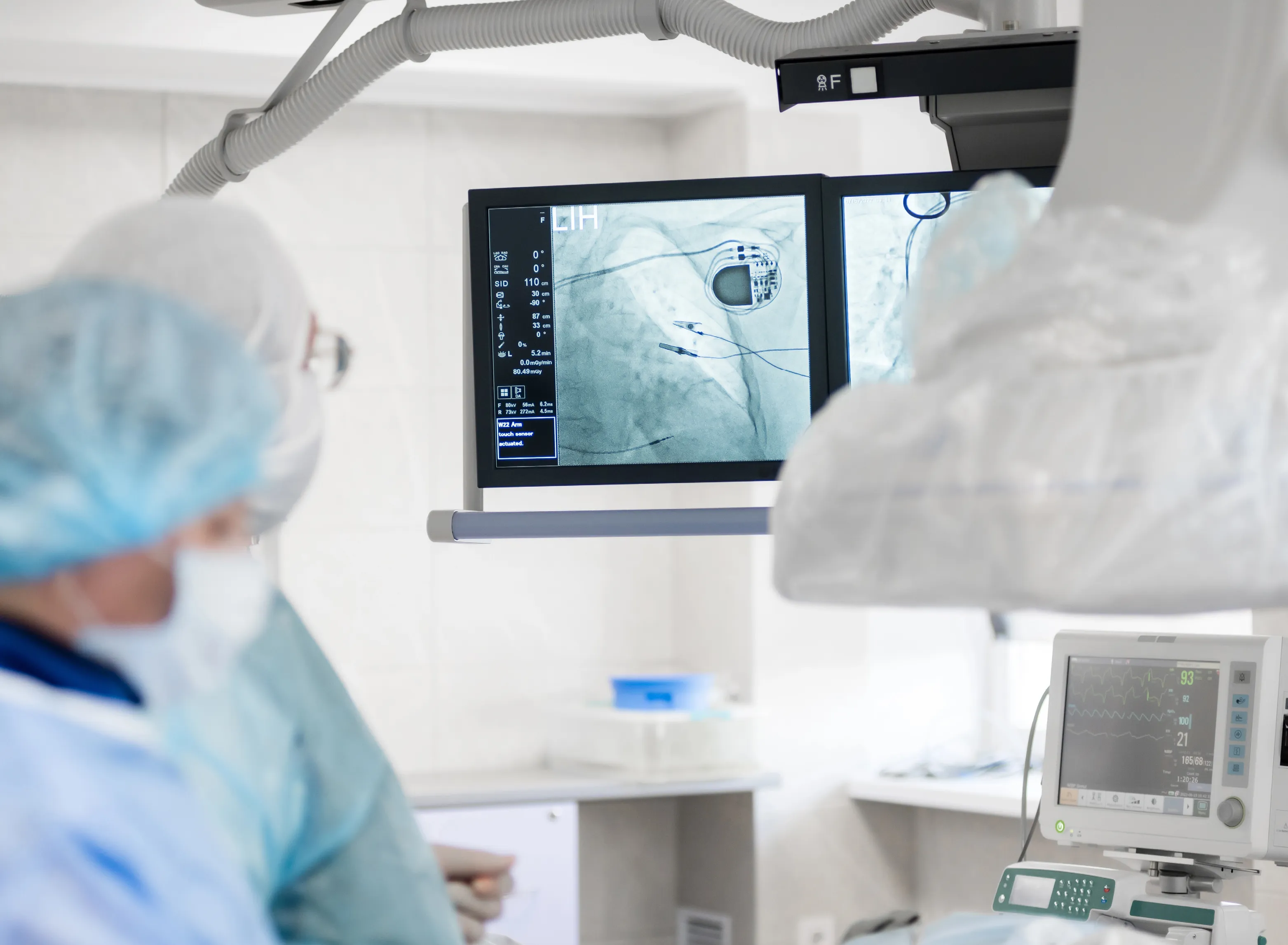
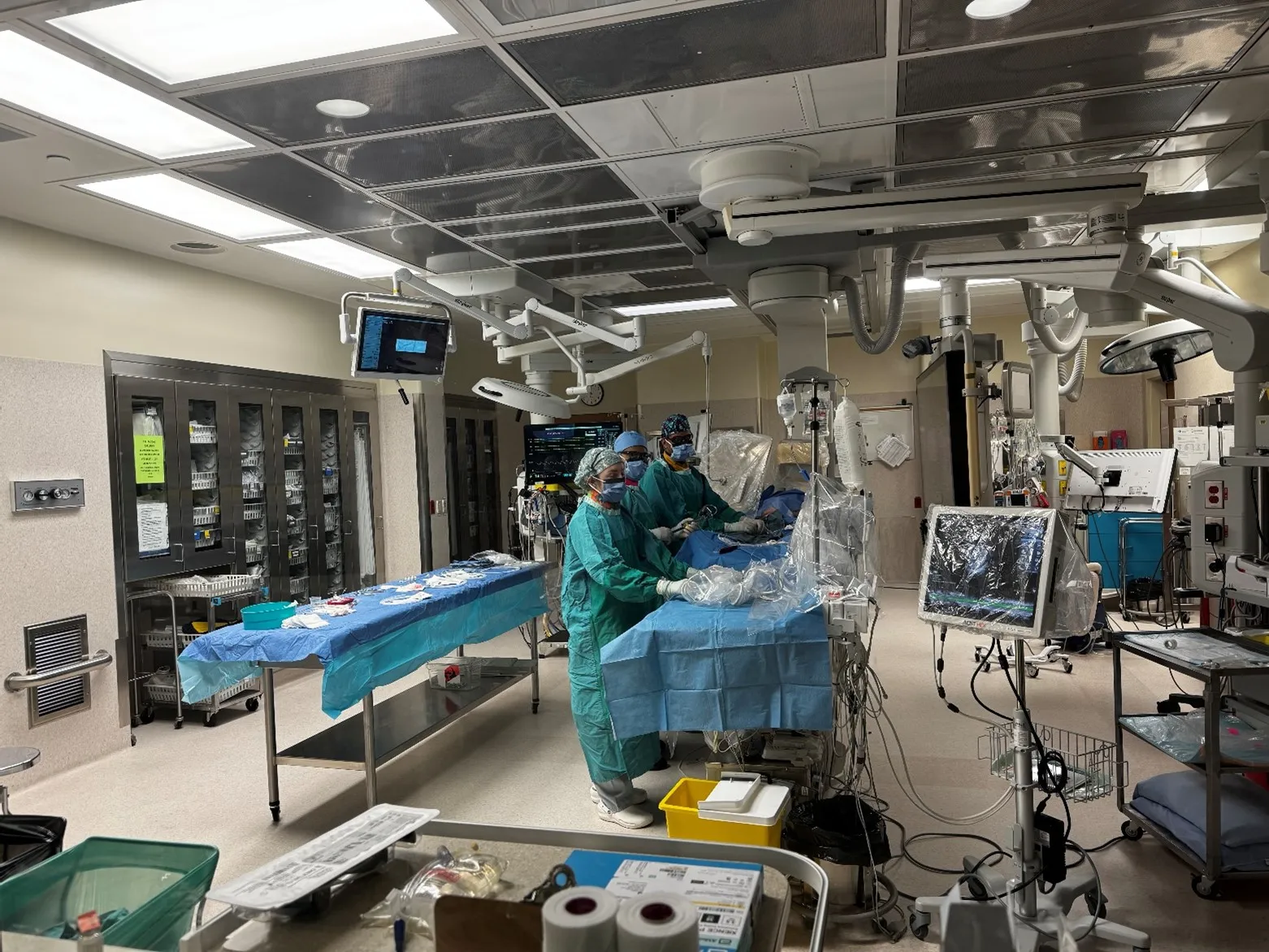
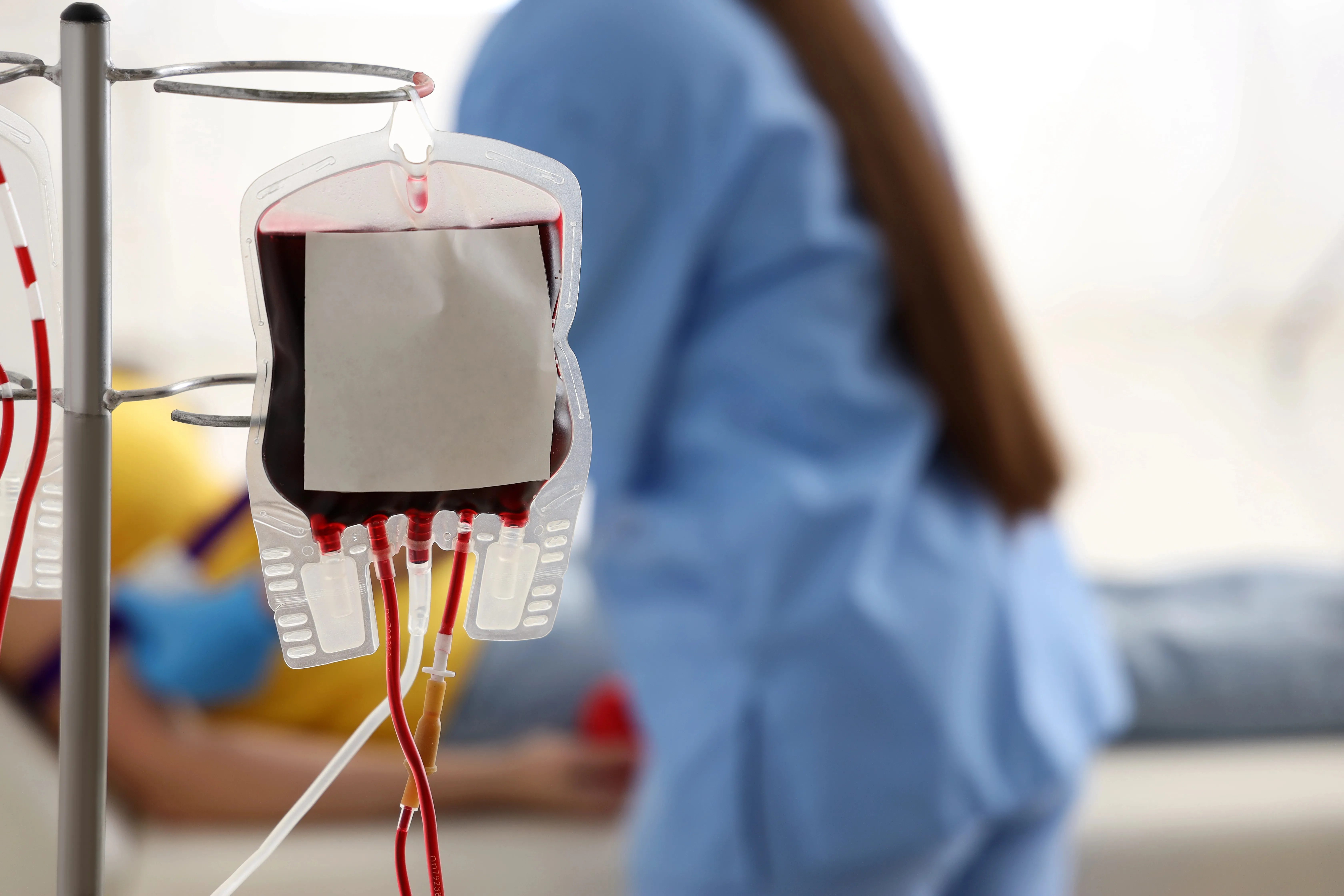
Welcome to the 2025 CVC Annual report, The Arteries of Innovation. Like all arteries, innovations have a beginning, a middle and an end, and the ideas–like red blood cells carrying oxygen–must flow through to the desired location. Our oxygen is the ideas that come from all parts, and ultimately flow to our patients when a discovery turns into a clinical innovation based on the most robust data available.
Given our Arteries of Innovation theme, we also think of the bench-to-bedside translation, including the population-wide observational data examinations led by Drs. Finlay McAlister and Padma Kaul. Without these data, we would not have the ability to generate or test new hypotheses and thus evaluate our storytelling with high-quality data.
This year saw important contributions from the CVC faculty. Our CVC family has grown and enriched our collaborative environment: Dr. Pishoy Gouda joined as our newest faculty member after pursuing further training with our colleagues at the Duke Clinical Research Institute. On the other end of the spectrum, our Co-Director, Dr. Padma Kaul, added to her accomplishments a Tier 1 Canada Research Chair in Women and Children's Cardio-Metabolic Health and launched several important studies in that growing (pun intended) sphere of clinical and population health research. Our future growth is also bright, as we welcomed trainees from across the globe to enhance their own research pathways as they developed new ideas.
In addition to ongoing population health, artificial intelligence, and clinical trial research, the CVC and its collaborators launched several studies that will shape future care. A few notable projects include the CIHR-funded AURORA study, which will examine type 1 diabetes, and the CFREF-supported One Child Every Child initiative, which will study perinatal and childhood environments and hopes to identify targets for future interventions. Further along the cardiovascular disease spectrum, the HEART Platform was launched (supported by University Hospital Foundation), creating a framework to study interventions for patients with acute and chronic heart failure. These studies complement the work ongoing in acute coronary syndromes (led by Drs. Kevin Bainey, Shaun Goodman, and Robert Welsh), pulmonary hypertension (led by Dr. Jason Weatherald), the interface with the kidney (led by Dr. David Collister), electrophysiology (led by Dr. Roopinder Sandhu), critical cardiovascular illness (led by Dr. Sean van Diepen), and prevention (led by Dr. Jacob Udell).
Please join us in reviewing the accomplishments of the CVC community and our network of collaborators, investigators, trainees, and patients, made possible by the generous research support of many organizations and individuals.